Cap on non economic damages in medical malpractice ruled unconstitutional by Florida Supreme Court
 In 2003 Florida lawmakers decided to limit non economic damages for negligence of practitioners to $500,000 or $1 million “if the negligence resulted in a permanent vegetative state or death”. At the time lawmakers said the cap would stop the medical malpractice insurance crisis and prevent doctors from leaving Florida. However there is no evidence of crisis Today and the Supreme Court of Florida recently ruled that this cap was unconstitutional.
In 2003 Florida lawmakers decided to limit non economic damages for negligence of practitioners to $500,000 or $1 million “if the negligence resulted in a permanent vegetative state or death”. At the time lawmakers said the cap would stop the medical malpractice insurance crisis and prevent doctors from leaving Florida. However there is no evidence of crisis Today and the Supreme Court of Florida recently ruled that this cap was unconstitutional.
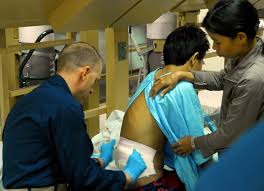
The ruling arose from the case of a victim of medical malpractice who saw the initial amount awarded by a jury substantially reduced by a judge based on this cap. Susan Kalitan had her esophagus perforated during an outpatient surgery for carpal tunnel syndrome. She spent 3 months in the intensive care unit including six weeks in a medically induced coma. She sued the North Broward Hospital District and other people involved in her care at the public district. She was initially awarded $4.7 million by the jury for pain and suffering. This amount was reduced to $1 million by Broward Circuit Judge Jack Tuter based on the cap described above. After the cap was found unconstitutional by the Fourth District Court of Appeals, the hospital appealed the decision. In a 30-page opinion the Supreme Court confirmed that the cap was unconstitutional.
Read more in Daily Business Review
 New York Personal Injury Attorneys Blog
New York Personal Injury Attorneys Blog



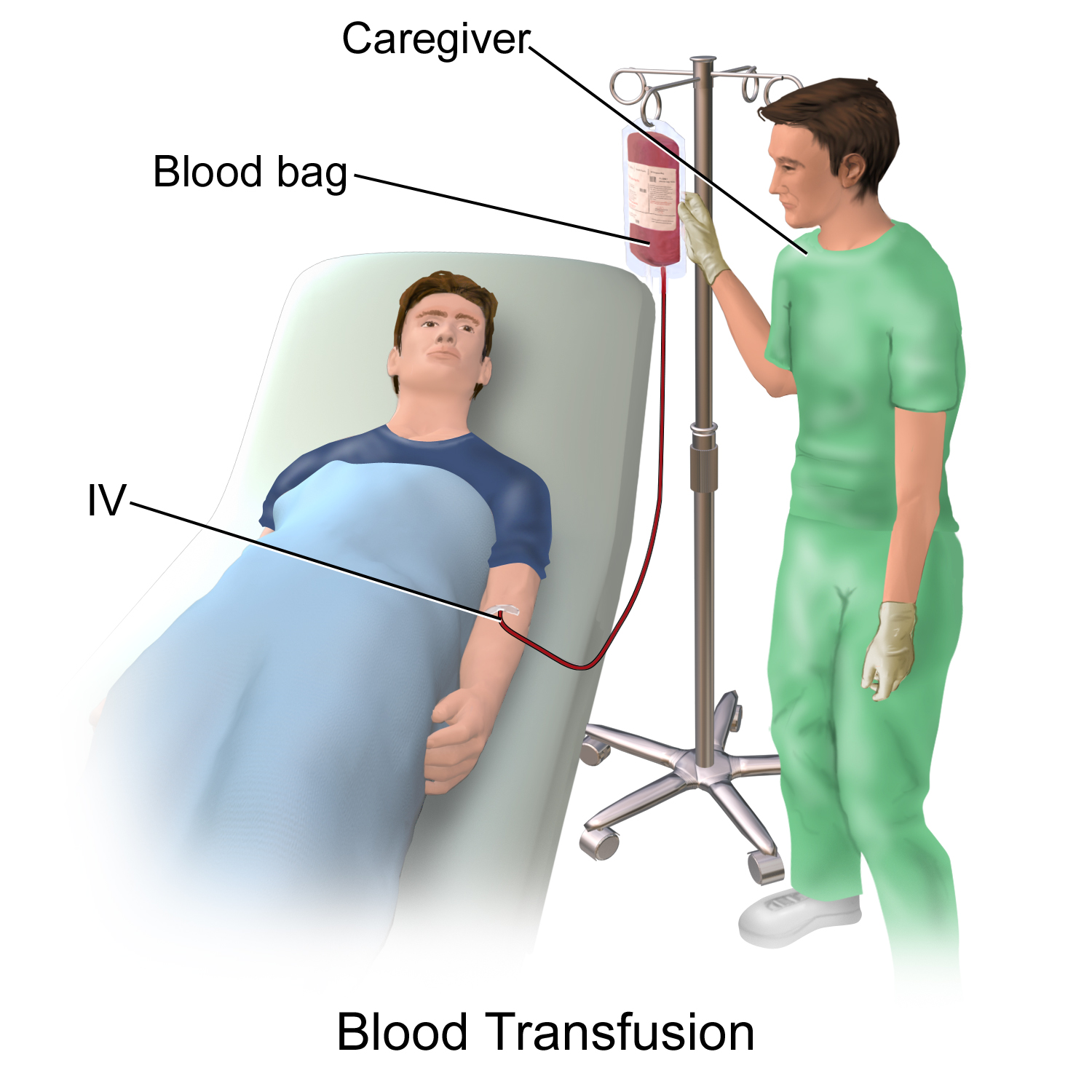 As healthcare providers implement new technologies and therapies every year, they also create unanticipated risks of medical malpractice. The
As healthcare providers implement new technologies and therapies every year, they also create unanticipated risks of medical malpractice. The  As healthcare evolves so does
As healthcare evolves so does 
 Medical Malpractice may have been committed on many American Africans who were previously diagnosed with hypertrophic cardiomyopathy. A recent study found that some genetic variations that were linked to this condition were indeed harmless. These specific genetic variations were found more often in black Americans than in white Americans. Therefore many patients from African descent may have been misdiagnosed or are still being
Medical Malpractice may have been committed on many American Africans who were previously diagnosed with hypertrophic cardiomyopathy. A recent study found that some genetic variations that were linked to this condition were indeed harmless. These specific genetic variations were found more often in black Americans than in white Americans. Therefore many patients from African descent may have been misdiagnosed or are still being